Fusidic acid: Uses, forms, and safety tips
Fusidic acid is a topical antibiotic many doctors prescribe for skin infections caused by Staphylococcus bacteria. It treats impetigo, infected eczema, boils, and infected wounds. You’ll find it as fusidic acid cream, ointment, or as oral sodium fusidate in some countries.
How fusidic acid is used
Apply a thin layer of cream or ointment to clean, dry skin once or twice daily as directed. Cover with a dressing only if your doctor tells you to. For impetigo, treatment often lasts 5 to 7 days; for deeper infections, oral treatment may be longer. Follow the prescription exactly and finish the full course even if the rash clears up.
Resistance and safety
Fusidic acid works well against many staph strains, but resistance can develop quickly when it’s misused. That's why doctors avoid using it alone for certain infections and prefer combining it with systemic antibiotics when needed. Avoid long-term or unnecessary use to help protect its effectiveness.
What to watch for: Local irritation like itching or burning can happen. Serious allergic reactions are rare but seek care for swelling, severe rash, or breathing problems. Oral use can cause gastrointestinal upset and, rarely, liver enzyme changes; your prescriber may check blood tests if you take it systemically.
Interactions and precautions: Topical fusidic acid has few drug interactions, but oral forms can interact with other antibiotics and medications that affect the liver. Tell your clinician about other medicines, liver disease, or pregnancy. Do not use on large areas of broken skin unless advised.
Buying and storage tips: Only use fusidic acid prescribed or recommended by a healthcare professional. Store cream and ointment at room temperature away from direct heat. Discard leftover or expired medicine rather than keep it for future use.
Alternatives: If fusidic acid isn't suitable, common alternatives include topical mupirocin or oral antibiotics such as flucloxacillin or cephalexin, depending on the infection and local resistance patterns. Your clinician will choose based on the likely bug and allergy history.
When to see a doctor: See your clinician if the infection worsens, spreads, shows pus, fever develops, or if there’s no improvement after the prescribed course. For recurrent skin infections, your doctor may test for carrier status or check for underlying causes like diabetes.
Simple application tips: Wash and dry the area first, apply a thin layer, then wash your hands. Avoid contact with eyes and mouth. If you also use a topical steroid, use them exactly as prescribed—some combined products exist but steroids can thin skin with prolonged use. Do not bandage unless instructed.
Pregnancy, kids, and tests: Topical fusidic acid is used in children but check dosing with a pediatrician. In pregnancy and breastfeeding, ask your doctor before using topical antibiotics. For recurrent or severe infections, your clinician may swab the skin to identify bacteria and check sensitivity.
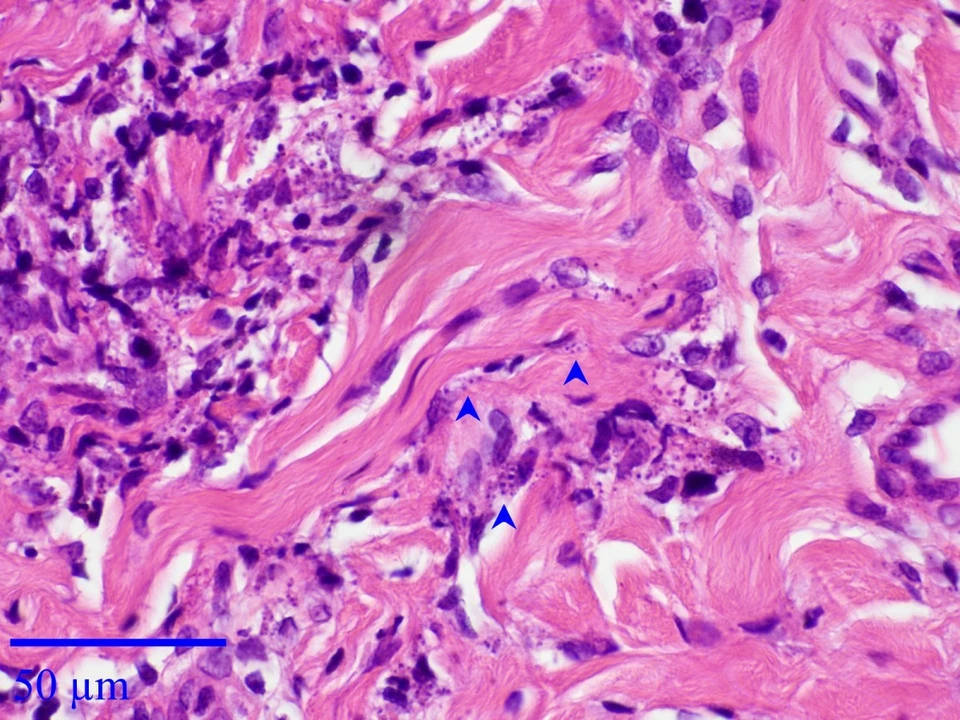
The Use of Fusidic Acid in the Management of Cutaneous Leishmaniasis
I recently came across an interesting study about the use of fusidic acid in managing cutaneous leishmaniasis. For those who may not know, cutaneous leishmaniasis is a parasitic skin infection that can cause severe skin lesions. Fusidic acid, commonly used for bacterial skin infections, has shown promise in treating this condition. The research indicates that it can be an effective and safe alternative to traditional treatments. This is great news for those affected by this infection, as it offers a new option for management and recovery.
About
Skin Care and Dermatology
Latest Posts


Acamprosate vs Alternatives: Which Alcohol‑Dependence Medication Works Best?
By Marcel Kornblum Sep 26, 2025

Generic Copays vs Brand Copays: Average 2024 Costs Explained
By Marcel Kornblum Jan 27, 2026

Nocebo Effect and Statin Side Effects: How Expectations Shape Your Experience
By Marcel Kornblum Jan 15, 2026