Switching Antibiotics: When and How to Do It Safely
Ever wondered when it’s okay to change antibiotics? You’re not alone. People switch drugs for a few clear reasons: bad side effects, allergic reactions, no improvement, lab results that point to a different bug, or needing to move from IV to pills. This guide tells you what to watch for and what to do next—without medical jargon.
Signs you should call your doctor now
If you get a rash, swelling, trouble breathing, or severe stomach pain after starting an antibiotic, stop the drug and seek emergency care. Those are signs of an allergy or a serious reaction. Also call if you get bloody or very watery diarrhea, a high fever that won’t drop, or if symptoms get much worse instead of better. For non-urgent issues—like nausea or a mild rash—contact your prescriber for advice before stopping anything.
How doctors decide to switch antibiotics
Most switches come from clear reasons. If cultures or tests show the bacteria are resistant, the doctor will pick a more effective drug. If you’re not better after 48–72 hours for many infections, they may change treatment. Another common switch is from IV antibiotics in hospital to an oral form once you can swallow and are improving. That’s called IV-to-oral conversion and helps you finish treatment at home.
When switching, prescribers consider allergies, kidney and liver function, drug interactions, pregnancy or breastfeeding, and infection location. For example, some antibiotics don’t reach the lungs well, others aren’t safe in pregnancy. Your current meds matter—some antibiotics raise the effect of blood thinners or interact with heart drugs.
Don’t stop an antibiotic without guidance. Stopping early can let bacteria survive and become resistant. If a doctor tells you to switch mid-course, they’ll usually give a clear new plan: which drug, for how long, and any monitoring needed.
Practical tips you can use now: keep a list of allergies and current meds, note when symptoms start and how they change, and bring that info to telehealth or clinic visits. Ask your provider: "Why are we changing this?" and "What side effects should I watch for?" Also ask if the new antibiotic needs dose changes for kidney problems or if you should avoid alcohol or certain foods.
Some switches aim to reduce broad antibiotic use. If tests show a narrow-spectrum antibiotic will work, doctors prefer that to lower the chance of resistance and side effects. That’s called de-escalation and is a common safe move once labs are back.
If you’re ever unsure, call your pharmacist or prescriber. They can confirm dosing, check interactions, and tell you what to expect. A careful switch can fix the problem without adding new ones—so get the right info and follow the plan.
Best Safe Alternatives to Amoxicillin: Expert Guide on Switching Antibiotics
Not every infection listens to amoxicillin. This guide digs into what to do when that go-to antibiotic fails or stirs up trouble. We’ll break down clinical advice on switching to safe alternatives, explore common complications that force the swap, and give you practical tips for a smooth transition. Get all the facts and strategies for finding the right replacement for amoxicillin. Stay ahead of bacterial resistance and protect your health with informed choices.
About
Health and Medicine
Latest Posts

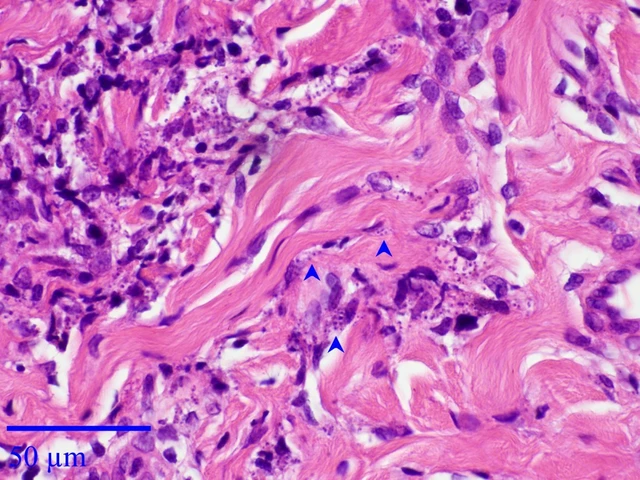
The Use of Fusidic Acid in the Management of Cutaneous Leishmaniasis
By Marcel Kornblum May 21, 2023

QD vs. QID: How Prescription Abbreviations Cause Dangerous Medication Errors
By Marcel Kornblum Mar 13, 2026

Parsnip Supplement Benefits in 2025: Gut Health, Blood Pressure, and Energy Explained
By Marcel Kornblum Aug 27, 2025

