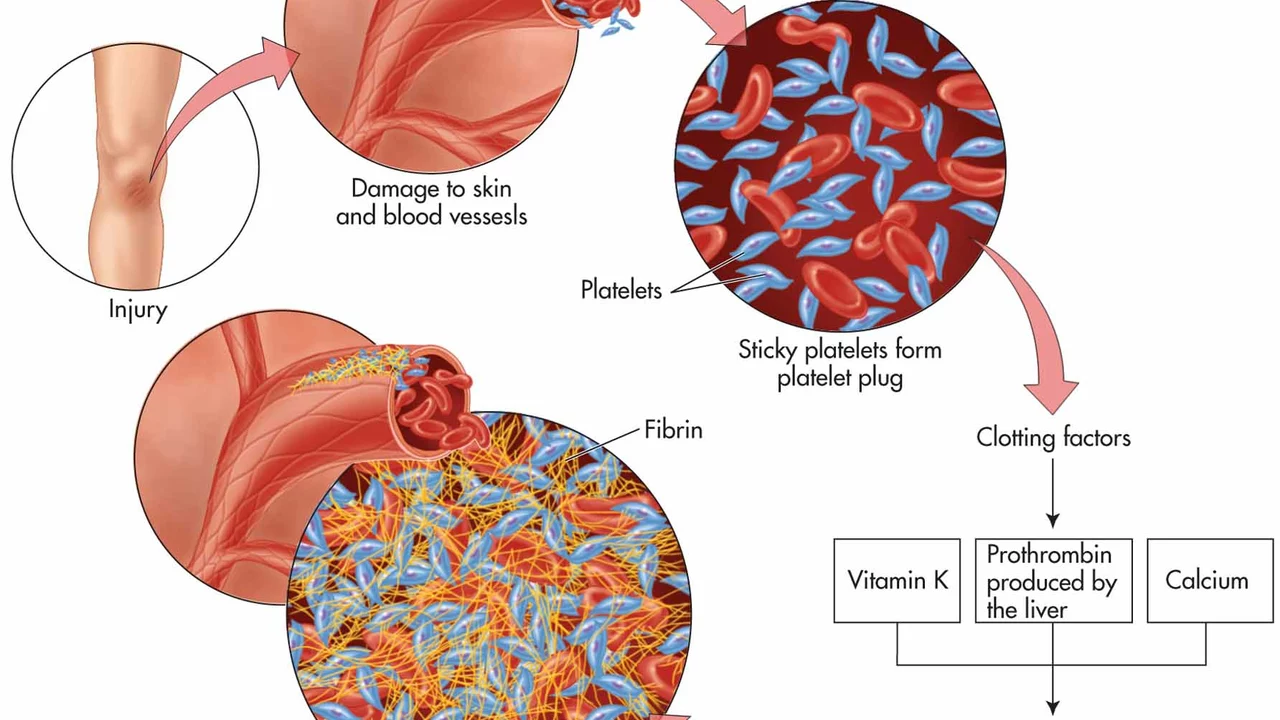
Blood clots: what to watch for and what to do
Blood clots can form quietly and become dangerous fast. Some clots stay in a leg or arm (deep vein thrombosis, DVT). Others break free and travel to the lungs (pulmonary embolism, PE) — that can be life-threatening. This page gives clear, actionable info so you know when to worry and how to reduce your risk.
Spotting a dangerous clot
Watch for sudden symptoms. For a DVT: one leg or arm becomes swollen, warm, and painful — often behind the calf. If you have chest pain, sudden shortness of breath, rapid heartbeat, fainting, or cough up blood, treat it as an emergency; those can be signs of a PE. Don’t wait for all symptoms; a single strong sign means call emergency services or get to urgent care.
Some people get clots with little pain. If you have risk factors — recent surgery, a long flight or car trip, active cancer, pregnancy or recent birth, or take blood-clotting drugs like estrogen-containing birth control or hormone therapy — be extra alert. A family history of clotting disorders raises risk too.
What doctors use to find and treat clots
Doctors start with a physical exam and may run a D-dimer blood test. For DVT they often use an ultrasound. For suspected PE they use CT pulmonary angiography. Treatment depends on location and severity. Most DVTs and PEs are treated with anticoagulants (blood thinners). These include newer direct oral anticoagulants (DOACs), low molecular weight heparin, or warfarin in some cases. In severe PE with instability, doctors may use clot-busting drugs or procedures.
How long you stay on a blood thinner depends on why the clot happened. A one-time event after surgery might need a few months of treatment. If you have an ongoing risk or a blood-clotting disorder, treatment can be longer. Always follow your doctor’s plan and attend follow-up tests.
Be careful with drug interactions. Some antibiotics like clarithromycin can affect warfarin levels. If you take blood thinners, tell every provider and pharmacist about them before new meds are started.
Prevention is often simple: move regularly on long trips, flex your feet and ankles, stay hydrated, avoid tobacco, manage weight, and follow your doctor’s advice after surgery. For people at higher risk, doctors may recommend compression stockings or short-term blood thinners around surgery or during long travel.
If you suspect a clot, don’t hesitate. Quick action saves lives. If you’re curious about how certain medications or conditions on this site relate to clot risk — for example antibiotic interactions or stroke risk after heart issues — check our related articles or ask your healthcare provider for specifics.
Got questions or a specific situation? Reach out to your clinician — or use this site’s contact page to learn which articles can help you prepare for a clinic visit.
The psychological impact of blood clots in stents: coping strategies and support
Dealing with blood clots in stents can take a toll on a person's mental health, leading to stress, anxiety, and even depression. The fear of complications, recurring health issues or undergoing surgery can be overwhelming. However, coping strategies like mindfulness, routine exercise, and maintaining a healthy diet can greatly help manage these concerns. Support from therapists, support groups, or loved ones is crucial in overcoming these psychological hurdles. It's important to remember that it's okay to seek help and take care of your mental health, as it plays a vital role in your overall well-being.
About
Health and Wellness
Latest Posts

The role of pharmacists in managing Ledipasvir therapy for Hepatitis C patients
By Marcel Kornblum Jul 16, 2023

Genetic Testing for Cancer Risk: BRCA, Lynch, and Beyond
By Marcel Kornblum Nov 27, 2025

Buy Cheap Generic Glucophage Online - Safe 2025 Guide
By Marcel Kornblum Oct 6, 2025