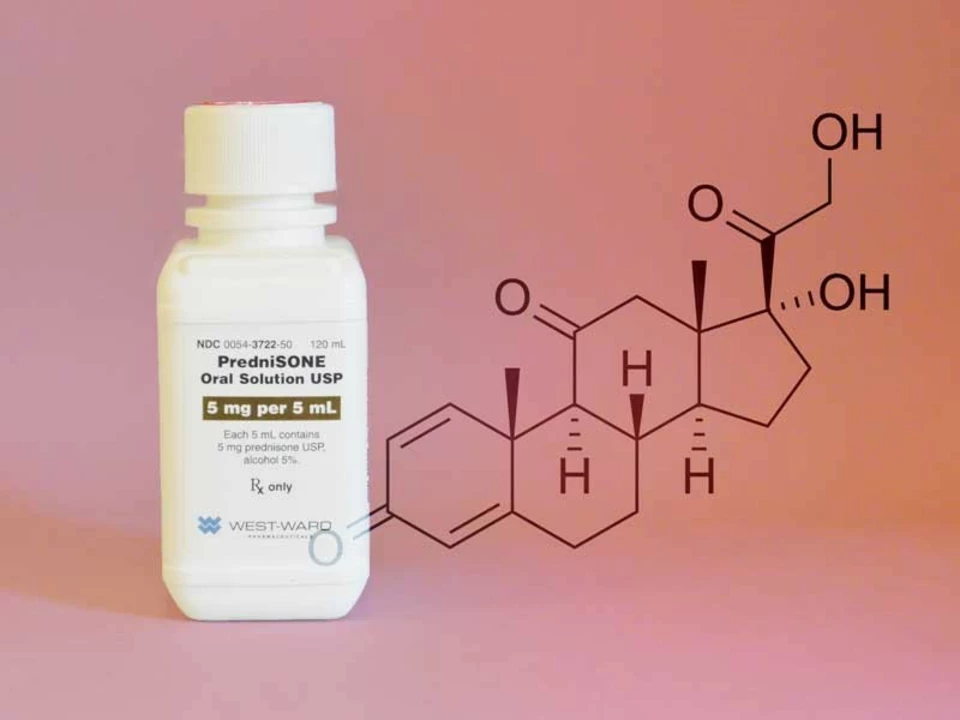
Prednisolone — what it treats and how to use it safely
Prednisolone is a steroid medicine doctors use for many inflammatory and immune problems: asthma flares, allergic reactions, some rashes, arthritis, certain eye and bowel conditions, and more. It works fast to calm inflammation, but it also affects lots of body systems. That’s why you need clear rules on dose, duration, and when to stop.
Short courses (a few days) can relieve sudden symptoms. Longer use raises more risks and needs planning — especially around infections, blood sugar, bone health, and mood.
Typical doses and how doctors decide
Dosing varies a lot by condition. For an acute flare you might see 5–60 mg a day depending on severity and body weight. For chronic conditions doctors aim for the lowest effective dose and may use alternate-day dosing to limit side effects. Always follow the prescription — don’t split or change doses on your own.
If you’ve been on prednisolone for more than 2–3 weeks, you usually need a taper (slow dose reduction). That prevents adrenal insufficiency, where your body can’t make enough natural steroid right away. Tapers depend on the starting dose and how long you’ve taken it; your prescriber will give a schedule.
Common side effects and what to watch for
Short-term side effects include increased appetite, trouble sleeping, mood swings, and higher blood sugar. Long-term use can cause weight gain, thinning skin, easy bruising, bone loss (osteoporosis), cataracts, and higher infection risk. If you have diabetes, check blood sugar more often while on prednisolone.
Serious signs that need fast medical attention: fever or signs of infection, severe stomach pain, sudden vision changes, chest pain, severe mood changes or suicidal thoughts, or signs of adrenal crisis such as extreme weakness, low blood pressure, fainting, or confusion.
Prednisolone interacts with many drugs (blood thinners, certain vaccines, diabetes meds, some antifungals and antibiotics). Tell your doctor about every medicine and supplement you take, and don’t get live vaccines while on significant steroid doses.
For bone protection, your doctor may suggest calcium, vitamin D, and bone-sparing meds if you need long-term treatment. Try to maintain weight-bearing exercise and avoid smoking and excessive alcohol.
Pregnancy and breastfeeding: doctors use prednisolone when benefits outweigh risks. It crosses the placenta less than some steroids, but discuss timing and dosing with your care team. Small amounts pass into breast milk; many experts still use it carefully if needed.
Storage is simple: keep tablets in a cool, dry place away from children. If you miss a dose, follow your prescriber’s advice — don’t double up unless instructed.
Questions? Talk to your doctor or pharmacist before starting or stopping prednisolone. If you notice new symptoms while on it, report them quickly — early action prevents complications.
Prednisolone vs. Prednisone: What's the Difference?
As a blogger, I've recently researched the differences between Prednisolone and Prednisone, two common corticosteroids used in treating various medical conditions. I discovered that while both medications are similar in their anti-inflammatory properties, the main difference lies in their respective forms. Prednisone is an inactive drug that requires conversion into Prednisolone by the liver to become active. This means that people with liver issues may not metabolize Prednisone as effectively, making Prednisolone a better choice for them. Ultimately, your doctor will determine the best medication for your specific situation, considering factors such as your medical history and the condition being treated.
About
Health and Medicine
Latest Posts

State Laws on Generic Drug Substitution: How Rules Vary Across the U.S.
By Marcel Kornblum Feb 18, 2026

How to Spot a Pharmacy Labeling Error Before Taking a Medication
By Marcel Kornblum Dec 21, 2025

Return to Work With Chronic Pain: Accommodations and Plans
By Marcel Kornblum Feb 26, 2026