Idiopathic Pulmonary Fibrosis (IPF): What You Should Know
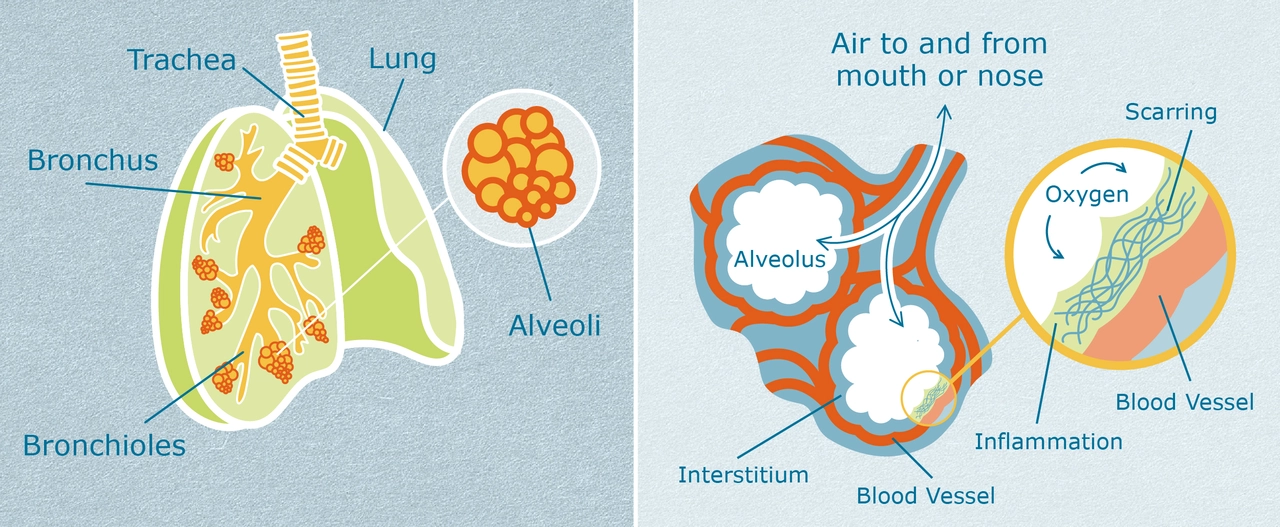
Idiopathic pulmonary fibrosis, or IPF, is a lung disease that causes scar tissue to build up in the lungs for no clear reason. That scarring makes it harder to breathe and to move oxygen into your blood. People usually notice gradual shortness of breath and a dry, persistent cough. IPF most often affects people over 60, and it tends to get worse over time.
How IPF is diagnosed
If you or your doctor suspect IPF, expect tests that focus on lung structure and function. A high-resolution CT (HRCT) scan is the main imaging test; it shows the pattern of scarring and “honeycombing.” Pulmonary function tests (PFTs) measure lung volume and gas transfer—watch for reduced FVC and DLCO. Your doctor may order blood work to rule out other causes, and sometimes bronchoscopy or a lung biopsy is needed when the picture isn't clear. Early referral to a pulmonologist experienced with interstitial lung disease (ILD) helps get the right diagnosis faster.
Treatment and day-to-day management
There’s no cure that reverses scarring, but treatments can slow progression and improve quality of life. Two antifibrotic drugs—pirfenidone and nintedanib—have been shown to slow the decline in lung function. Oxygen therapy helps if your blood oxygen falls, especially during activity or sleep. Pulmonary rehab (supervised exercise and breathing training) often improves stamina and reduces breathlessness.
Other practical steps matter too. Stay up to date on flu and pneumonia vaccines. Stop smoking and avoid secondhand smoke. Treat acid reflux if present—some people with IPF do better when GERD is controlled. If you qualify, discuss lung transplant with a specialist early; transplant can be lifesaving for selected patients. Also ask about clinical trials—new treatments are being studied all the time.
Know the warning signs that need quick attention: sudden worse shortness of breath, fever, chest pain, or confusion. These could mean a complication like infection, blood clot, or an acute IPF flare and may require urgent care.
Living with IPF means planning ahead. Work with your care team on an action plan for flares, keep a list of medications and oxygen prescriptions, and discuss advance care preferences while you're well enough to make clear decisions. Palliative care can help manage symptoms and improve daily comfort even while you continue active treatments.
IPF can feel overwhelming, but the right team and early steps can make a real difference. If you have persistent breathlessness or a chronic dry cough, talk to your primary doctor and ask for a pulmonology referral. Timely diagnosis opens more treatment options and support.
The Impact of Idiopathic Pulmonary Fibrosis on Relationships and Social Life
Living with idiopathic pulmonary fibrosis (IPF) has significantly affected my relationships and social life. The constant fatigue and breathlessness make it difficult to engage in activities with friends and family, leading to feelings of isolation. The unpredictability of my condition also causes stress and anxiety for my loved ones, as they worry about my health. To cope, we've had to adapt our communication and find new ways to connect, like through video calls or online games. Overall, IPF has taught me the importance of cherishing the moments I have with my loved ones and seeking their support during tough times.
About
Health and Wellness
Latest Posts


8 Alternatives to Wellbutrin Sr
By Marcel Kornblum Feb 28, 2025

Buy Cheap Generic Claritin Online - Safe, Fast & Affordable
By Marcel Kornblum Oct 5, 2025
The role of pharmacists in managing Ledipasvir therapy for Hepatitis C patients
By Marcel Kornblum Jul 16, 2023